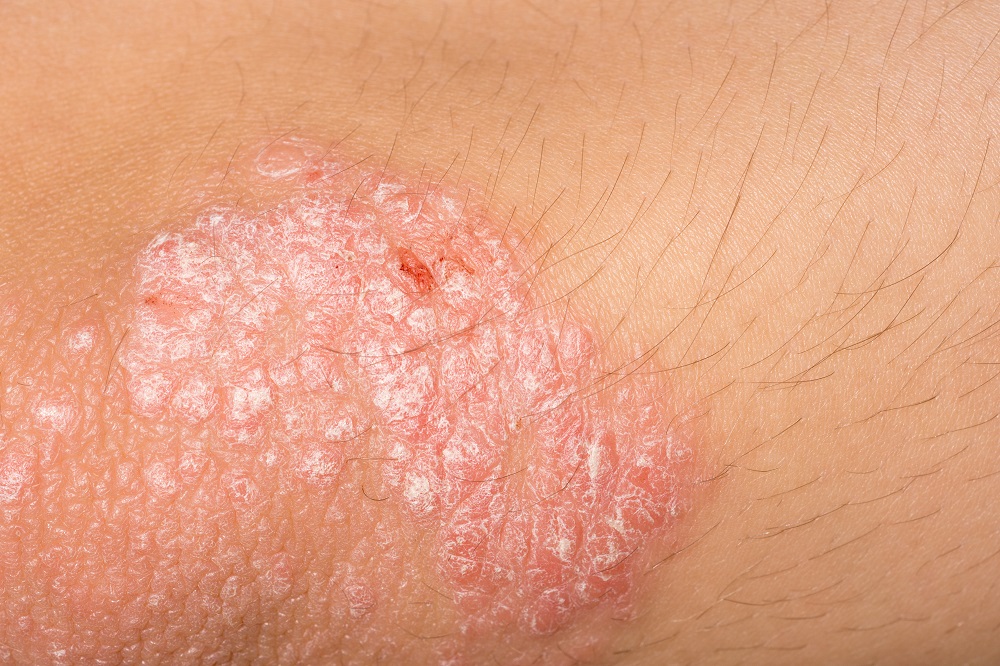
Psoriasis symptoms may vary from person to person. However, it includes one or more of the following signs:
- Red skin patches covered with silvery scales (a few spots or major eruptions covering a large area)
- Small scaling spots
- Dry, cracked skin that sometimes bleeds
- Itching
- Burning
- Pain
- Thickened, pitted or ridged nails
- Stiff joints
- Swollen joints
- Flakes of dead skin in the hair or on the shoulders, especially after scratching the scalp
- Small, water-drop-shaped sores on trunk, arms, legs and scalp
- Smooth patches of red, inflamed skin
- Pitted, discolored nails
Most types of psoriasis go through cycles: After having flared for a few weeks or months, they then may subside for some time, or even go into complete remission.
There are various types of psoriasis, such as:
- Plaque psoriasis (most common): The patients have dry, raised, red skin lesions covered with silvery scales. The plaques (just a few or many) itch or might be painful and can occur anywhere on the body.
- Nail psoriasis: This type can affect finger- and toenails. It results in pitting, abnormal nail growth and discoloration. The nails might even become loose, separate from the nail bed or crumble.
- Scalp psoriasis: It appears as red, itchy area with silvery-white scales. Affected people may notice flakes of dead skin in their hair or on their shoulders, particularly after scratching their scalp.
- Guttate psoriasis: For the most part, this psoriasis affects children and young adults, and is normally triggered by a bacterial infection, e.g. strep throat. The small, water-drop-shaped sores on trunk, arms, legs and scalp are covered by a fine scale. It either occurs as a single outbreak that disappears on its own, or as repeated episodes.
- Inverse psoriasis: This type affects the skin in the armpits, groin, under the breasts and around the genitals, and causes smooth patches of red, inflamed skin that gets worse by friction and sweating. Fungal infections may trigger inverse psoriasis.
- Psoriatic arthritis: Mild to severe psoriatic arthritis doesn’t only result in inflamed, scaly skin but also in pitted, discolored nails and swollen, painful joints (in any place). This type may cause stiffness and progressive joint damage that in the most serious cases might lead to permanent deformity.
The cause of psoriasis isn't fully known, but it's thought to be related to an immune system problem with cells in the body. However, experts believe that at least ten percent of the population inherits one or more of the genes that create a predisposition to the disease. But only two to three percent of the population develops psoriasis. It seems that the individual that finally develops the disease must have a combination of the genes that cause it and in addition, he/she has to be exposed to external factors (triggers).
Triggers / risk factors for psoriasis
- Stress
- Smoking
- Heavy consumption of alcohol
- Extreme overweight
- Sunburns
- External skin irritations
- Streptococcus infection
- Certain medications (e.g. high blood pressure medications such as beta blockers, antimalarial drugs, and iodides)
People that suffer from psoriasis are at greater risk of developing certain diseases, such as:
- Psoriatic arthritis
- Obesity
- Kidney disease
- Type 2 diabetes
- High blood pressure
- Cardiovascular disease
- Metabolic syndrome
- Eye disorders (e.g. conjunctivitis, blepharitis and uveitis)
- Other autoimmune disease (e.g. celiac disease, sclerosis, inflammatory bowel disease)
- Parkinson's disease
Psoriasis may also increase the risk of:
- Low self-esteem
- Depression
- Social isolation
- Problems at work, which can result in lower income
Those factors might have a negative impact on the quality of life.
Medical Treatment
The dermatologist normally diagnoses psoriasis by checking skin, scalp and nails after having gained information on the medical history of the affected person. Psoriasis is not contagious, but there is a hereditary tendency. Therefore family history is helpful in making the diagnosis. Rarely, the doctor takes a small skin sample to rule out other disorders (e.g. seborrheic dermatitis, lichen planus, ringworm of the body, pityriasis rosea).
Psoriasis treatments have the goal to stop the skin cells from growing quickly, which reduces inflammation and plaque formation, as well as remove scales and smooth the skin. It’s important to find the right treatment together with the dermatologist because what works for one person might not work for another.
Treatment options:
- Topicals: They are applied to the skin and are mostly the first treatment to try after the diagnosis. Topicals normalize or slow down excessive cell reproduction and reduce psoriasis inflammation. Steroids (corticosteroids) are the most frequently used treatment for the disease. They are anti-inflammatory agents, because they reduce the swelling and redness of lesions. Anthralin, synthetic vitamin D3, and vitamin A are also prescribed to control psoriasis lesions.
- Light therapy: The skin is exposed to ultraviolet light under medical supervision and on a regular basis.
- Biologics: Biologic drugs are used for moderate to severe psoriasis and psoriatic arthritis that has not responded to other treatments. They are administered by injection or intravenous (IV) infusion.
- Systemics: Systemic medications are taken orally or administered by injection. The drugs work throughout the body. They are usually given to patients with moderate to severe psoriasis and psoriatic arthritis.
- New Oral Treatments: The symptoms are supposed to improve by inhibiting specific molecules associated with inflammation. These treatments can be taken as tablets.
- Complementary and alternative medicine: These medical and health care systems, practices and products aren’t considered to be part of Western medicine. They focus more on preventative care and pain management. Examples: acupressure, acupuncture, reiki, massage, meditation, aromatherapy, spa therapy, yoga, tai chi, anti-inflammatory diet.
Preventive measures
Psoriasis cannot be prevented because the exact causes that lead to the disease are still not fully understood. But by observing themselves, the affected people may detect factors that trigger a new attack or aggravate psoriasis. It gives them the opportunity for trying to avoid them.
Self-help measures may include:
- Quit smoking
- Reduce alcohol intake
- Reduce stress
- Lose weight
- Take a shower or bath with care
- Keep in mind that:
- Dry skin makes irritation and itchiness worse
- Too many baths and showers can strip the skin of natural oils
- Plain water may dry the skin
- Hot water can irritate the skin
- Rubbing the skin with a towel can worsen the condition
- Keep in mind that:
Therefore:
- Don’t bathe every day, especially during the winter months
- Use lukewarm water
- Add oil, salts, or finely ground oatmeal to bath water after having soaked for a minute to soothe the skin
- Pat yourself dry
- Then apply cream on a regular basis (consistency is very important)
- Use a moisturizer regularly, e.g. thick ointments, such as vaseline, olive oil, heavy skin creams (not too much ointment on hot summer days)
- Areas with psoriasis: before going to bed, wrap the slathered-up skin with a bandage, and wash the area gently in the morning (can reduce scaling)
- But too much moisturizer on hot days may worsen the psoriasis
- Get some sun but avoid sunburn
- Cover the areas of the skin without psoriasis with a sunscreen lotion, SPF of 30 or higher
- Start with twenty minutes a day for 3 days a week
- Some medicines aren't safe when combined with lots of sun, so talk to your doctor first
Treatment of psoriasis in Germany
Dermatological clinics (acute care clinics) »
Dermatological clinics (university hospitals) »