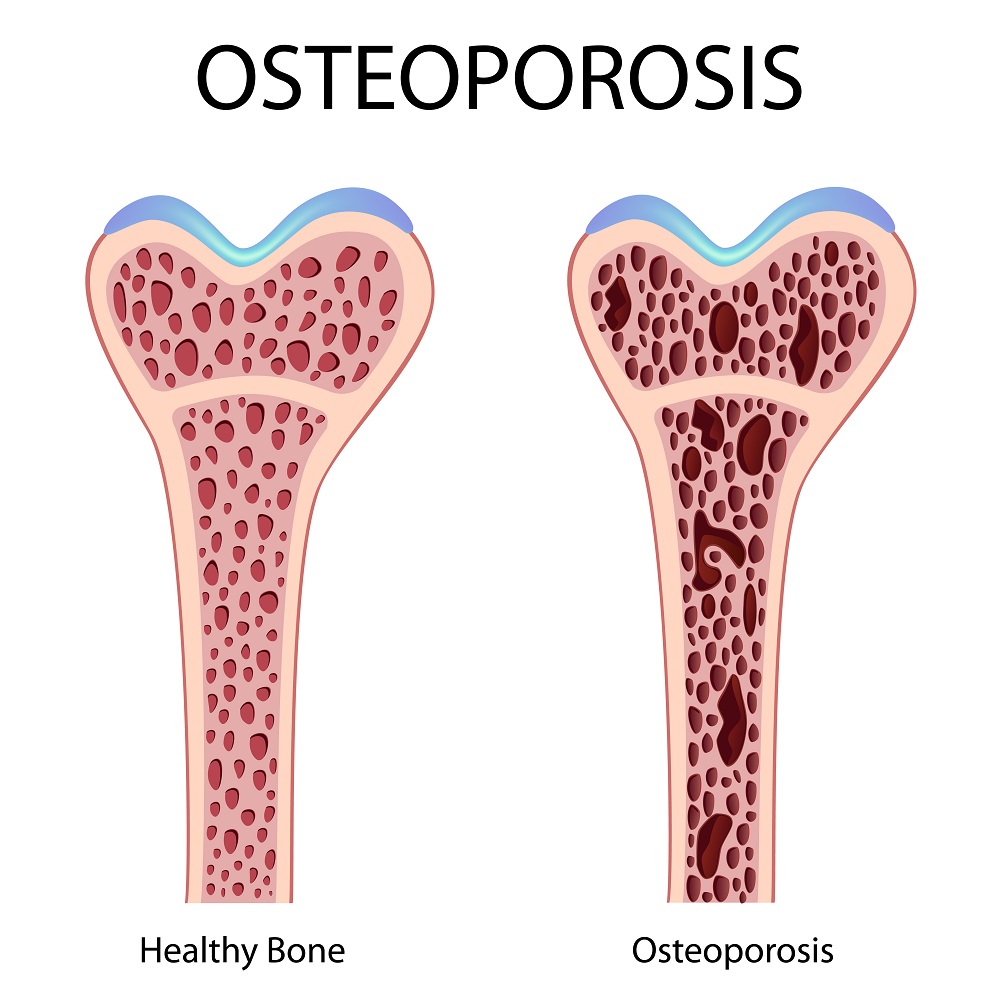
Osteoporosis often starts with no signs. But once bones have been weakened by the disease, symptoms may include:
- Tense muscles
- Backache
- Severe back pain
- Gradual loss of height
- Stooped posture
- Fractures of the spine, hip or wrist
Bones are in a permanent state of renewal – new bones are made and old bones are broken down. The body of a teenager makes new bone quicker than it breaks down old bone, and the bone mass increases. Usually, people reach their peak bone mass by their early 20s. But older people lose their bone mass faster than it's created, e.g. when estrogen levels decline in the menopause. The bones become weak, which can lead to osteoporosis. How likely somebody develops osteoporosis depends partly on how much bone mass he/she attained in the youth. The higher the peak bone mass, the less likely the person develops osteoporosis as he/she ages.
Risk factors for osteoporosis
- Gender: higher risk for women
- Age: higher risk for older people
- Women over the age of 50 are at the highest risk (they have lighter, thinner bones)
- Bone structure and weight: higher risk for thin and small-boned women and men because they have less bone to lose than people with more body weight and larger frames
- Family history: higher risk for people with parents or grandparents who have/had signs of osteoporosis
- Prior history of broken bones
- Smoking
- Heavy alcohol use (may result in thinning of the bones)
- Other diseases, e.g. rheumatoid arthritis
- Certain medications, e.g. steroids such as prednisone
Bone fractures, especially in the hip or spine, are the most serious complications of the disease. Hip fractures are often caused by a fall and may result in disability and even death from postoperative complications, especially in older people. But spinal fractures might also occur if the patient hasn’t fallen. The vertebrae may weaken to the point that they crumple and lead to back pain, lost height and a hunched forward posture.
The physician can measure the bone density by a machine that uses low levels of X-rays to determine the proportion of mineral in the bones. Usually, only the bones in the hip, wrist and spine are checked.
Treatment depends on the risk estimate of breaking a bone in the next ten years. If the risk is low, the patient might not get medication and treatment may focus on lifestyle, safety and modifying risk factors for bone loss.
Bisphosphonates
For people at increased risk of fracture, the most widely prescribed medications are bisphosphonates. But they have side effects, such as nausea, abdominal pain or difficulty swallowing. Intravenous forms don't lead to stomach upset. If the therapy goes on for more than five years, it may result in more serious problems but a doctor can give advice on how to proceed.
Hormone-related therapy
There are a few hormone-related therapies that help increase bone density:
- Estrogen: If a female patient starts with estrogen right after menopause, it may help maintain bone density. But this therapy can also increase her risk of getting blood clots, endometrial cancer, breast cancer or a heart disease. Therefore, the doctor usually suggests estrogen for bone health only if the patient’s menopausal symptoms also have to be treated.
- Raloxifene (Evista): It mimics the positive effects of estrogen on bone density in postmenopausal women – without having some of its risks. Using this drug might also reduce the risk of a few types of breast cancer. Side effects are hot flashes and an increased risk of blood clots.
- Testosterone: Testosterone replacement therapy may help increase bone density, but since osteoporosis medications have been better studied in men with osteoporosis, they are recommended alone or in addition to testosterone.
There are more medications, especially for patients that cannot tolerate the more common treatments for osteoporosis or in case the therapy doesn’t work well. The doctor might suggest Denosumab (Prolia) that reduces the chance of all types of fractures, or Teriparatide (Forteo) that stimulates new bone growth.
Preventive measures
It’s important to keep the bones healthy throughout the life by:
- Taking adequate amounts of calcium
- Between ages of 18 and 50: 1,000 milligrams per day
- Women over 50: 1,200 milligrams per day
- Men over 70: 1,200 milligrams per day
- Good sources of calcium include:
- Low-fat dairy products
- Dark green vegetables (e.g. broccoli)
- Mineral water
- Soy products, e.g. tofu
- Calcium-fortified orange juice and cereals
- Calcium supplements may help get enough calcium but the daily dose of calcium should not exceed 2,000 milligrams for people over 50
- Taking adequate amounts of vitamin D
- Improves the body's ability to absorb calcium
- Adequate amounts may be acquired from sunlight but there is an increased risk of getting skin cancer
- Good alternative: vitamin D supplement
- Recommended daily dosage for older adults with low blood levels of vitamin D: 20 μg or around 1,000 international units (IU)
- Teens and other adults can take up to 4,000 IU per day
- The fat-soluble vitamin is preferably taken with the main meals
- Exercising on a regular basis
- For strong bones and slow bone loss
- Beneficial: combination of strength training (for stronger muscles and bones in arms and upper spine) and weight-bearing exercises
- Jogging, walking, stair climbing, skiing as well as impact-producing sports: affect muscles and bones in legs, hip and lower spine
- Good cardiovascular workout: cycling, swimming, exercising on machines (cross trainer) – however, these low impact exercises are not so helpful regarding bone health