- Group A (also Streptococcus pneumonia)
- Via inhalation of droplets of secretions from throat and nose, when an infected person coughs or sneezes
- Via contact with infected wounds or sores on the skin
- Normally not through casual contact
- Quite often in crowded environments (e.g. dorms, schools, etc.)
- Risk of infection usually stops 24-48 hours after antibiotic treatment has started
- Group B
- Via vaginal secretions during vaginal delivery to newborn baby
- Viridans
- Inhabit the mouth of healthy people
- May invade the bloodstream, e.g. in people with periodontal inflammation, and infect heart valves
Symptoms depend on the site of infection:
- Cellulitis: red, infected skin with swollen, painful tissue underneath
- Impetigo: highly contagious bacterial skin infection most common among preschool children
- Scabby, yellow-crusted sores
- Necrotizing skin infections: connective tissue covering muscle is infected
- Chills, fever, severe pain, tenderness in the affected area
- Skin might appear normal until infection gets worse
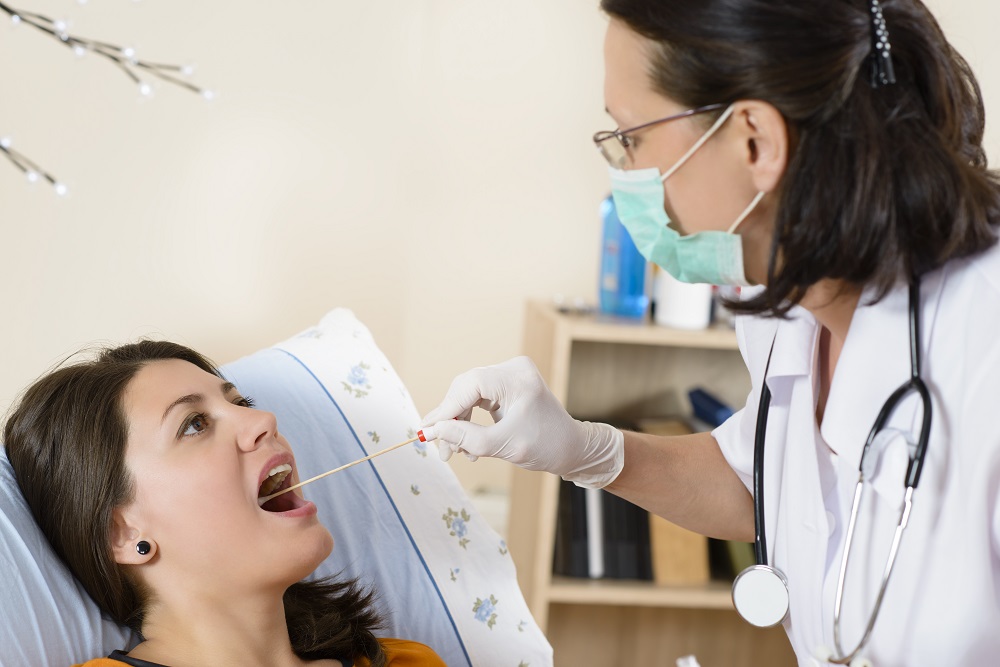
- Strep throat that normally affects children 5 to 15 years old
- Symptoms often occur suddenly
- Red, sore throat
- In children: chills, fever, headache, nausea, vomiting, malaise
- Swollen tonsils with or without patches of pus
- Enlarged and tender lymph nodes in the neck
- In children under three years: sometimes only a runny nose
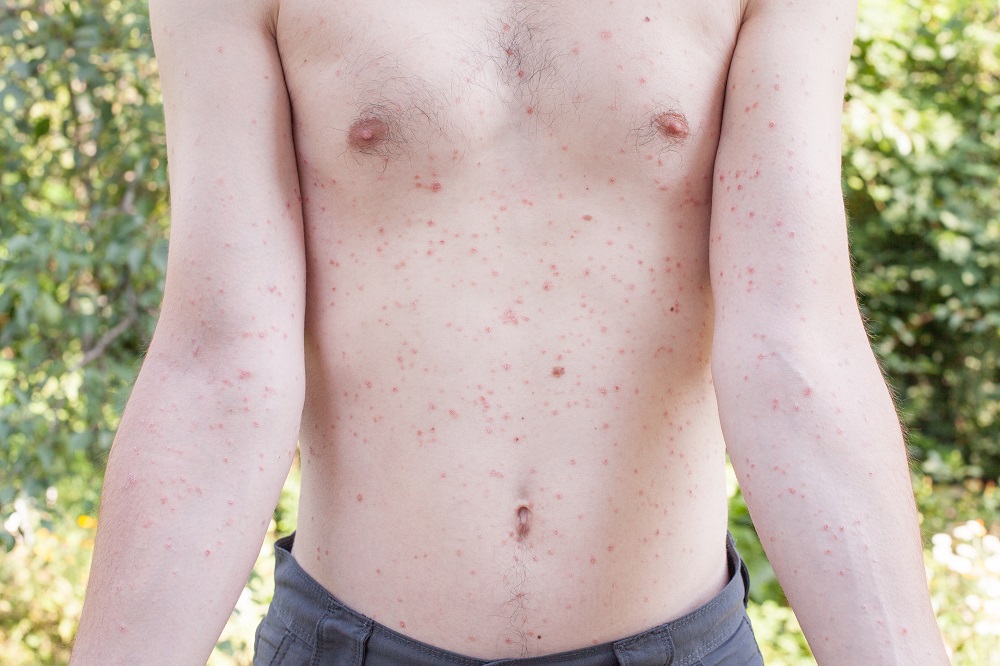
- Scarlet fever
- Starts with a rash on the face
- Spreads to the trunk and limbs
- Rash is worse in skinfolds
- Skin peels when rash fades
- On the tongue: red bumps with a yellowish white film. When the film peels, tongue appears beefy red
Many species of streptococci live harmlessly in and on the body. A few species that can cause infection are also present in some healthy people but cause no symptoms. However, an infection with streptococcus often happens through airborne droplet infection or by direct physical contact with another infected person. Living together in crowded environments, close contact and poor hygiene are also likely to favor the infection. The different groups of these bacteria are spread in different ways, e.g. via sneezing, coughing, contact with infected sores, during vaginal delivery (from mother to child).
If the infection is not treated, the person may remain infectious for between ten and 21 days. An untreated infection with a pus-filled discharge might remain infectious for months. Medication should be taken as prescribed, and it’s important to complete the course of antibiotics.
However, if untreated, streptococcal infections can result in problems. Some complications are caused by the spread of the infection to nearby tissue, e.g. an ear infection may spread to the sinuses (sinusitis). Moreover, some people develop kidney inflammation or rheumatic fever.
Medical Treatment
Usually the streptococcal infection is treated with antibiotics (almost always Penicillin) that kill the bacteria. For necrotizing fasciitis, surgery is needed to remove dead tissue. As for strep throat, it normally resolves within one to two weeks, even without treatment.
However, antibiotics shorten the duration of symptoms in young kids but have only a small effect on signs in teenagers and adults. Nevertheless, antibiotics are given to prevent the spread of the disease to the middle ear, sinuses, and mastoid bone, as well as to prevent spread from person to person. The treatment also helps prevent rheumatic fever.
Preventive measures
Maintaining good health and hygiene may reduce the risk of bacterial infection. The spread of bacteria might be prevented by not sharing food or eating utensils, washing hands frequently, and cleaning and bandaging scrapes and cuts.